The Link Between Personality and Immunity
It’s easy to see how personality could influence a person’s health in general. An impulsive person might head to a party instead of getting a good night’s sleep. A careless person might not wash the hand that just held onto a subway pole during flu season. A responsible person might grab that wool hat before heading out into the cold. But when it comes to how the body handles an illness, you probably expect your antibodies to stir into action with complete objectivity — all character traits aside. In other words, it’s a lot harder to see how personality could influence a person’s immune function in particular.
Yet during the past 20 or so years, psychological scientists have uncovered a great deal of evidence supporting that very connection. This emerging line of study linking personality and immunity remains in its initial stages and has produced mixed results. Nevertheless, researchers have found that several basic personality markers — extraversion, hostility, and optimism among them — do seem to play a role in how well someone wards off sickness. Simply put, the body’s ability to rouse its natural defenses may depend, at least in part, on the mind’s particular disposition.
“Personality has to do with how people think, feel, and behave,” says Suzanne C. Segerstrom of the University of Kentucky, “and all of those qualities can affect biological signals like neurotransmitters and hormones that influence the immune system for better or worse.”
A Sociable Cure for the Common Cold
APS James McKeen Cattell Fellow Sheldon Cohen of Carnegie Mellon University is one of the leading researchers on personality and immunity. He recalls stumbling onto this connection almost by accident. He and some collaborators were studying the effects of interpersonal relationships on immune function and thought to include personality as a control variable. In the end, however, some of these stable character traits turned out being predictors of immunity themselves.
“We just wanted to be sure we weren’t looking for personality, when in some cases it turns out that at least to some degree we were,” says Cohen.
Eventually the researchers decided to investigate personality and immunity outright. For one study, published in a 2003 issue of Psychological Science, Cohen and others recruited several hundred people through newspaper ads who agreed to let the researchers give them rhinovirus — otherwise known as the common cold. (The scientists did make it worth the while of study participants, giving them $800 in compensation.)
Before the participants were exposed to the illness, the researchers performed all sorts of tests to determine their baseline immune function and personality traits. Cohen and company specifically wanted to measure “sociability,” which they defined as a combination of extraversion, agreeableness, and personal relationships. Leading up to the quarantine, participants completed sociability questionnaires and also kept a six-day diary of social interactions.
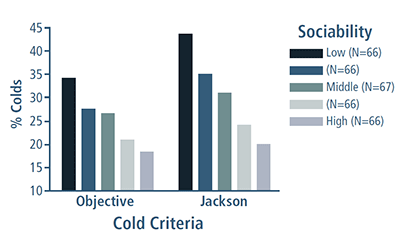
In their 2003 paper “Sociability and Susceptibility to the Common Cold” in Psychological Science, Cohen et al. found a rate of developing colds (adjusted for controls) as a function of sociability quintile. Colds were defined either as infection plus objective signs of illness or as infection plus subjective symptoms of illness (modified Jackson Scale).
Finally the day arrived for the participants to be inoculated with rhinovirus. For several days afterward, the researchers documented various cold symptoms (congestion, runny nose, sneezing, sore throat, and the like) and collected mucus samples for testing. A month later, the researchers ran a blood test for antibodies as a further measure of participant immune function. All told, about a quarter of the participants contracted a legitimate cold.
When Cohen and collaborators analyzed the data, they found that as sociability increased, the rate of illness decreased. Put another way, the simple fact that some people were naturally less sociable seemed to make them naturally less capable of fighting off the cold. The clear-cut relationship held true whether the cold was measured through objective signs (like mucus) or subjective ones (like symptoms).
The connection between sociability and immunity persisted even when the researchers controlled for eight potential variables. Demographic factors like age, race, and education didn’t impact the relationship, nor did biological factors like a person’s preexisting antibody function. The fact that sociability was measured before the illness would seem to eliminate reverse causation — that the cold was causing someone to be less sociable.
The character trait of sociability itself was apparently running the immunity show. “So more sociable people tend to have better immune function in our work,” says Cohen. In other work — some of it reviewed in a 2006 paper in Current Directions in Psychological Science — he and collaborators found that trait positive affect made a person less likely to develop a cold, too.
“It was kind of accidental for both of those areas,” says Cohen. “But we’ve gone on to replicate that work and show that these are very stable effects.”
When Positivity Trumps Negativity
Positive character traits do seem to enhance a person’s immune resistance. In addition to helping the body fight a cold, extraversion (one of the key elements of sociability) has been associated with higher lymphocyte counts in older people and with a lower rate of viral load in HIV patients. Trait positive affect, meanwhile, has been linked to lower production of inflammatory cytokines — a likely sign of a strong immune response.
Negative personality traits also seem to have an effect on immunity in some cases. Neuroticism has been a fairly consistent predictor of antibody response to vaccines, for instance, though it seems unrelated to the development of a common cold. Hostility, meanwhile, has been a reasonably reliable indicator that a person will produce more inflammatory cytokines, though again not every study of this relationship has found a significant link.
“What’s fascinating is, when I first came into the field, everyone thought the brain and the immune system were pretty separate — that they functioned in many ways independently,” says Anna L. Marsland of the University of Pittsburgh. “Now we really understand that it’s absolutely not the case, and that they’re very closely tied to one another.”
While both positive and negative dispositions appear to play a role in immune function, some of Marsland’s recent work suggests that positivity may be the more powerful factor. In one study from several years ago, Marsland and collaborators (including Cohen) gave 84 healthy graduate students a series of hepatitis B vaccinations. Five months after the first dose was administered, and shortly after the second shot, the researchers drew blood to measure the antibody response. They reported in a 2001 issue of Health Psychology that participants with higher trait negative affect showed a less protective immune reaction.
A little while later, Marsland and the same collaborators reanalyzed the data, this time shifting their focus from negative disposition to trait positive affect. Upon this closer inspection, they realized that they’d emphasized the wrong personality characteristic the first time around. In a subsequent paper, published in a 2006 issue of Brain, Behavior, and Immunity, the researchers reported that test participants with more positive dispositions were the ones who mounted greater antibody responses to the vaccine. What the original work had shown was really the absence of an upbeat personality, not the presence of a negative one. Once positive affect was entered into the model, the independent association between negative affect and immunity disappeared.
“For a long time people were really focused on negative affect and negative emotions,” says Marsland. “There’s this slightly newer literature that’s looked at stable positive affect. Individuals who tend to see things in a more positive way — there might be health benefits of that.”
“Little” Versus “Big” Traits
The personality traits measured by Cohen and Marsland tend to be rather fixed; they’re sometimes called “big” characteristics. But some aspects of personality can shift a bit depending on various events and scenarios, and these so-called “little” traits seem to have an impact on immunity, too. In fact, Segerstrom has found the effects of “big” and “little” personality to be completely opposed at times, with “big” optimism predicting weak immune response, for instance, and “little” optimism predicting a strong one.
“Personality doesn’t have to be conceptualized as perfectly stable traits or types,” says Segerstrom. “It can be situation-specific and vary across situations.”
For one recent study, Segerstrom and a collaborator followed 124 first-year law students to measure how their personalities shifted during this grueling year, and to see if their immune responses changed as a result. At five points during the year — beginning before the semester began and ending when students interviewed for critical summer law internships — the researchers administered personality questionnaires and a DTH (delayed-type hypersensitivity) skin test. The DTH test measured an immune response known as cell-mediated immunity, or CMI.
Segerstrom focused on optimism as a follow-up to her previous work on that personality trait. Participants completed questionnaires specifically designed by Segerstrom to measure optimism in law students (one item, for example, was, “I will be less successful than most of my classmates”). For the CMI test, participants were first injected with an antigen (either a mumps virus or a candida yeast), then given the DTH skin test two days later. Positive and negative affect were also measured as potential complicating variables.
When Segerstrom and her collaborator analyzed the data, they found that as a person’s optimism toward the law program increased, the immune response as indicated by CMI increased along with it. Conversely, when law-school optimism decreased, CMI decreased, too. Positive affect accounted for some of the optimism-immunity relationship, but only partially; negative affect didn’t seem to play a role.
The findings represent the “first evidence that expectancy change correlates with immunological change,” the authors concluded in a 2010 issue of Psychological Science.
Segerstrom says the study definitely reflects “little” optimism because it measured levels of expectation within a single person across various moments in time. The idea that optimism can be both a rather stable personality trait and also a flexible one makes sense. At the start of the year, when students had little to go on besides their LSAT scores, law-school optimism was mostly the product of a person’s general disposition. As class rankings were publicized over the course of the year, however, expectations could understandably change even within a generally optimistic person.
“This kind of complexity … is where the literature on personality is heading,” says Segerstrom, referring to the fact that two different types of optimism might have different effects in the same person. “Or, if not, it should be.”
Finding Pathways and Potential Interventions
Cohen believes the next step for the field should be to identify the mechanisms that facilitate the personality-immunity connection. “I think we just know so little right now about personality and immunity,” he says. “What we need to do, if this is an area we want to pursue, is think more about what personality characteristics we would think would influence immunity, and through what pathways.”
Though the precise pathways by which personality puts its imprint on immunity remain a bit of a mystery, a number of possibilities have emerged. On the biological side, immune cells have receptors for neurotransmitters from the nervous system. The body’s hormonal systems — particularly the hypothalamic-pituitary-adrenal axis — offer another physiological avenue through which neural messages can reach the immune system.
Then there are behavioral pathways through which personality might influence immunity, too. A conscientious person, for instance, is more likely to refrain from smoking, which in turn has a known positive impact on immunity. A hostile person, on the other hand, may have a greater tendency to initiate social conflicts, which could introduce potentially harmful health factors into the equation. Things like diet, exercise, and sleep all depend, at least in part, on a person’s character.
And of course there are always potential genetic gateways that could conceivably contribute to both personality and disease susceptibility. Once these pathways are better understood, then in theory it should be possible to design treatments that boost the immune function of people with certain dispositions. Stable character traits are very hard to change, of course, but that doesn’t rule out the possibility of behavioral or pharmaceutical interventions. Simply teaching a hostile person to control his or her aggression, for instance, could have measurable trickle-down effects on the immune system.
“I’m not sure you can change these underlying dispositions, but I think you can hand people a number of types of skill sets to help them cope better with situations that may translate to decreased health risk,” says Marsland. “My take on this is that the jury’s out. We don’t know at this point. But most of us in the field are pretty optimistic that you can intervene at some level.”
References
Cohen, S., Doyle, W. J., Turner, R., Alper, C. M., & Skoner, D. P. (2003). Sociability and susceptibility to the common cold. Psychological Science, 14, 389–395.
Cohen, S., & Pressman, S. D. (2006). Positive affect and health. Current Directions in Psychological Science, 15, 122–125.
Cohen, S., Janicki-Deverts, D., Crittenden, C. N., & Sneed, R. S. (2012). “Personality and Human Immunity,” pp. 146–169. In Segerstrom, S. (Ed.). The Oxford Handbook of Psychoneuroimmunology. Oxford University Press.
Marsland, A. L., Cohen, S., Rabin, B. S., & Manuck, S. B. (2001). Associations between stress, trait negative affect, acute immune reactivity, and antibody response to hepatitis B injection in healthy young adults. Health Psychology, 20, 4–11.
Marsland, A. L., Cohen, S., Rabin, B. S., & Manuck, S. B. (2006). Trait positive affect and antibody response to hepatitis B vaccination. Brain, Behavior, and Immunity, 20, 261–269.
Segerstrom, S. C. (2006). How does optimism suppress immunity? Evaluation of three affective pathways. Health Psychology, 25, 653–657.
Segerstrom, S. C., & Sephton, S. E. (2010). Optimistic expectancies and cell-mediated immunity: The role of positive affect. Psychological Science, 21, 448–455.





Comments
Sociability and extraversion may have their effects because such individuals have more exposure to other people (and their illnesses). This may be a similar effect to people who are outdoors/work in the dirt more–they have better immune systems because of this increased exposure.
APS regularly opens certain online articles for discussion on our website. Effective February 2021, you must be a logged-in APS member to post comments. By posting a comment, you agree to our Community Guidelines and the display of your profile information, including your name and affiliation. Any opinions, findings, conclusions, or recommendations present in article comments are those of the writers and do not necessarily reflect the views of APS or the article’s author. For more information, please see our Community Guidelines.
Please login with your APS account to comment.