It’s flu season. Watch your prejudices.
I tried not to breathe too much on the elevator this morning. I was trying to avoid the germs of a fellow who clearly had the flu—or at least a nasty cold. There seems to be a lot of sickness going around right now, and I’m just being prudent. I know it would have been rude to cover my face or turn my back to this guy, so I just held my breath for the 10-story ride.
That’s my behavioral immune system kicking in. Behavioral immune system is just a fancy way of summarizing what the mind and body have long known, that one of the most powerful tools we have for staying well is to watch out for sick people, and then give them wide berth. Our ancient ancestors learned this lesson well, and it’s now entwined in our basic perceptions and thinking and decision making. It’s like a sentry, always vigilant for anything out there that’s suspicious.
But the system is not simple, nor is it infallible. First of all, it’s closely tied to our biological immune system—all those cells that detect and attack foreign invaders. What’s more, it’s far from perfect at recognizing what is a real health threat and what is not. Two new studies, both published on-line in the journal Psychological Science, explore this complex dual defense system, both its cleverness and its liabilities.
It’s been known for some time that our heightened vigilance can trigger a biological response as well. We’re heading into flu season now, so we’re primed to be circumspect, and this in turn puts the body’s disease-fighting cells on high alert. But does it also work the other way around? Two psychological scientists—Saul Miller of the University of Kentucky and Jon Maner of Florida State—suspected that it might, for this reason: The cellular immune system is imperfect. It causes an inflammatory response to fight off pathogens, but since this inflammatory reaction is harmful to tissue, it immediately produces anti-inflammatory cells to protect the body. Thus, after fighting off one disease, the body becomes susceptible to other infections for a short period of time. Miller and Maner had the idea that the initial immune response might trigger the behavioral immune system to provide extra protection during this time of vulnerability.
They tested this idea by dividing a group of volunteers into those who had been ill recently, and who had not. Then they very rapidly flashed photographs of people’s faces, some normal and others disfigured in some way. People who have contagious illnesses often appear abnormal—redness, swelling, tearing, scabs and sores—and those abnormalities are warning signs. The scientists reasoned that the mind’s imperfect detection system would also respond to other forms of disfigurement, unrelated to contagion.
And that’s just what they found. The recently ill volunteers—presumably with immune cells on alert—were much more likely to notice and pay attention to signs of facial abnormality. In other words, recent illness sparked a biological immune response which—independent of conscious concerns about illness—biased the volunteers’ attention to warning signs of contagion.
Of course, it’s was a mistaken response, so that’s not good. Indeed, it’s seriously wrongheaded, because the disfigured people in the photos were not sick at all. They just looked different. The skewed attention was prejudicial in a cruel and unfair way. And it gets worse. In a second experiment, the scientists measured not just attention, but actual avoidance. Again, they compared recently ill and healthy volunteers, but this time they used a joystick to gauge their automatic, unconscious approach or avoidance responses to disfigured people. And as predicted, the recently ill volunteers were much more avoidant. They responded automatically—but wrongly and prejudicially—to disease cues.
What’s novel here the first empirical evidence that activating the body’s immune cells shapes both cognition and behavior. Apparently our two immune systems are constantly backing each other up, providing additional lines of defense. But what about those disturbing social biases inherent in the behavioral immune system? The fact that this over-generalized prejudice is rooted in biology does not make it less of a concern; indeed, more. Is there any way to weaken this ancient, misguided response?
A second study suggests there might be. University of Toronto psychological scientist Julie Huang and her colleagues wondered if modern advances in immunology might also shape behavior, especially these irrational forms of prejudice. They decided to test the notion that public health measures like vaccines and hand washing might diminish vigilance for contagion, and in the process attenuate unfair social biases. In other words, if the physical threat of sickness can be eliminated, is it possible that the prejudicial thoughts and actions might also be eliminated?
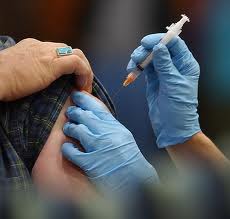 To test this, Huang and colleagues recruited volunteers during the height of the 2009 H1N1, or swine flu, epidemic. They had only half of the volunteers read a passage about swine flu, its severity, and a shortage of the highly recommended vaccine. All of the volunteers then indicated whether or not they had been vaccinated, and in either case they rated the effectiveness of the vaccine.
To test this, Huang and colleagues recruited volunteers during the height of the 2009 H1N1, or swine flu, epidemic. They had only half of the volunteers read a passage about swine flu, its severity, and a shortage of the highly recommended vaccine. All of the volunteers then indicated whether or not they had been vaccinated, and in either case they rated the effectiveness of the vaccine.
To measure prejudice, all the volunteers completed a scale that assesses attitudes toward immigrants. Even though there is no obvious connection between contagion and immigrants—as there is between contagion and disfigurement—fear of illness has been shown to trigger such irrational animosity. As it did here: Those threatened by the swine full did show an anti-immigrant bias, but only if they had not been vaccinated. Those who had been immunized—especially those who believed in its effectiveness—were much less prejudicial toward foreigners.
These are provocative findings, and the scientists wanted to double-check them in a different manner. In another experiment, some of the volunteers used a hand-wipe to wash their hands, while others did not. Then all the volunteers read the same passage about H1N1, only in this case the passage emphasized the effectiveness of anti-bacterial hand-wipes. Then they rated their impressions of nine social out-groups, including the obese, crack addicts, disabled people and immigrants. These attitudes were conflated into an overall attitude toward out-groups. And again, those concerned about the flu—but who had not had the opportunity to wash their hands—were likely to make the mental leap from germ aversion to social prejudice. But those who had taken measures to protect themselves against the flu had much more favorable views of people unlike themselves.
So a vaccine against prejudice? Perhaps, in a way. Vaccines and hand-washing are already recognized as cost-effective strategies for reducing sickness and death. Social prejudice is also detrimental to emotional and physical health. So such public health initiatives, the scientists suggest, might easily be turned into dual-purpose interventions for the enhancement of well-being.
Wray Herbert’s book, On Second Thought, is now out in paperback. Excerpts from his two blogs—“We’re Only Human” and “Full Frontal Psychology”—appear regularly in The Huffington Post and Scientific American.





APS regularly opens certain online articles for discussion on our website. Effective February 2021, you must be a logged-in APS member to post comments. By posting a comment, you agree to our Community Guidelines and the display of your profile information, including your name and affiliation. Any opinions, findings, conclusions, or recommendations present in article comments are those of the writers and do not necessarily reflect the views of APS or the article’s author. For more information, please see our Community Guidelines.
Please login with your APS account to comment.